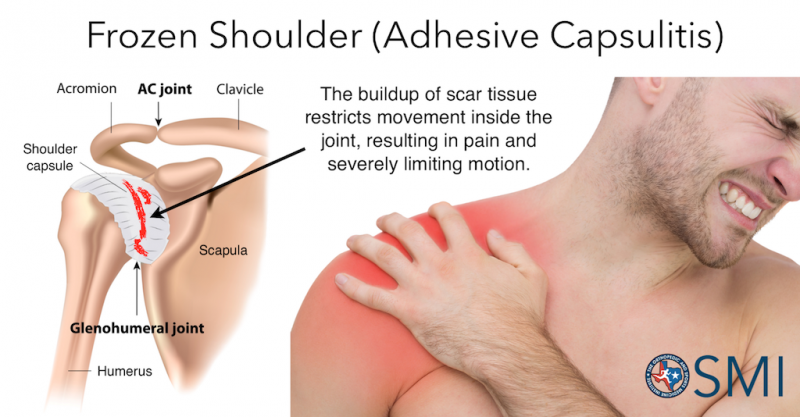
Frozen shoulder, also known as adhesive capsulitis, is inflammation of the entire shoulder capsule and joint. This process is generally characterized by three different stages; freezing, frozen and thawing. These stages describe progressive pain and stiffness that restrict patients from moving the joint. The shoulder joint is a ball in socket joint that is formed by the scapula and humerus, also known as the glenohumeral joint. This joint is surrounded by a capsule and filled with synovial fluid. The capsule is fused with surrounding tendons and ligaments that cause further complications if patients adopt a sedentary lifestyle. In any of these stages patients will experience pain and limitation raising their arms overhead; most limitations with shoulder external rotation, then abduction, followed by internal rotation. Frozen shoulder is typically a shoulder girdle issue that consists of tightness, weakness and lack of proper movement patterns.
So what causes frozen shoulder? In short, the lack of proper movement patterns cause tightness and hardening of the capsule. These movements tend to be accompanied with a sedentary lifestyle and poor posture. In the freezing stage, which ranges from 6 weeks to 9 months, patients have the first signs of tightness and pain. After sitting for an extended amount of time, joints have reduced circulation and blood flow. These changes affect the entire body starving certain joints of vital nutrients. Add poor posture to the equation and patients adopt an increased kyphotic posture resulting from tighter pec minor muscles and decreased mid back and rotator cuff strength.
Frozen shoulder occurs in stages. The best time to treat patients is as early as possible, before the damage progresses to the frozen stage. Once in this stage limitations last 4 to 6 months. Treatment in this stage can be painful for patients especially when breaking down the adhesion’s to regain proper movement patterns. The thawing stage ranges from 6 months to 2 years and is described as continued improvement in flexibility and strength of the shoulder. Patients will experience more function and may report feeling as though the arm is back to normal.
The main goals for treatment are to reduce pain, increase strength and improve movement. After regaining the proper shoulder mobility, attention should then be drawn to proper sitting posture to prevent further kyphosis of the spine. To keep the integrity of the shoulder is why you activate the mid back and keep the rotator cuff muscles strong. Lack of scapular stability can lead to excessive wear and tear and inflammation of the glenohumeral joint. Physical therapy is a great option to help heal acute and chronic pain, restore flexibility and strengthen all muscles needed to regain shoulder function.
So what do you do? The best option at home for acute pain is to apply ice for 10- 20 min, rest that shoulder and seek treatment with a physical therapist. Here you will be evaluated by a physical therapist and given a treatment plan depending on your specific needs. You can expect a combination of soft tissue mobilization, strengthening, and a home exercise routine to restore the proper movement pattern leading you to less pain, increased function and getting you back to your daily routine. Call (703) 723-9355 for an appointment with one of our many chiropractors, physical therapists, and acupuncturists that can help!