Sciatica is one of those scary, poorly understood words that I hear a lot of patients bring up. Sometimes it sounds like you get it just like you’d get the flu. “I caught that sciatica doc, there’s no more hope for me!” As it turns out, most patients don’t really have sciatica, and very commonly we can treat these patients successfully without drugs or surgery once they are accurately diagnosed.
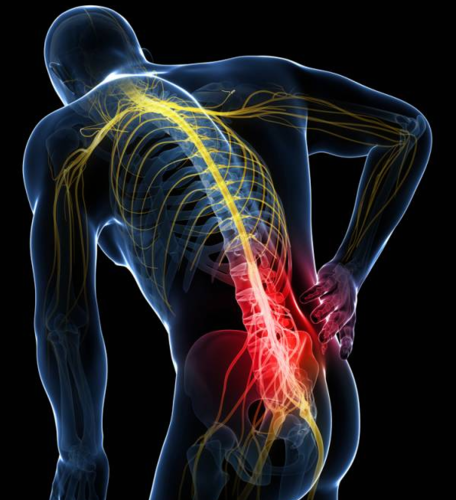
So, what is sciatica? First, let’s go over the sciatic nerve. All of the nerves that go to our arms and legs come from our spine. In the lower back, a large number of the spinal nerves, after exiting the spine, join together to form the ‘sciatic nerve’. This sciatic nerve runs down the buttock and back of the thigh and also innervates the entire lower leg and foot. This is why ‘sciatica’ is often used to describe pain going from the low back down into the buttock, hamstring, calf, or foot. Sciatica is specifically an irritation of the sciatic nerve that occurs as the nerve travels under a muscle called the piriformis in the hip. The old adage is, the piriformis gets tight, pushes on the sciatic nerve, and boom – pain.
nerves, after exiting the spine, join together to form the ‘sciatic nerve’. This sciatic nerve runs down the buttock and back of the thigh and also innervates the entire lower leg and foot. This is why ‘sciatica’ is often used to describe pain going from the low back down into the buttock, hamstring, calf, or foot. Sciatica is specifically an irritation of the sciatic nerve that occurs as the nerve travels under a muscle called the piriformis in the hip. The old adage is, the piriformis gets tight, pushes on the sciatic nerve, and boom – pain.
What’s the problem with that? Well for starters the piriformis doesn’t cause low back pain. If the muscle is tight, it can refer pain to the hip, thigh, and calf, but NOT up to the low back. Secondly, the actual chance of having true compression of the sciatic nerve is very low. Anatomically speaking, less than 2% of people are at risk of the piriformis causing direct compression; it’s a rare anatomical variant called piriformis syndrome. Thirdly? Reviews of the literature clearly demonstrate that the prevalence of true ‘sciatica’ among those presenting to primary care doctors with low back pain is less than 5% – pretty slim odds. There’s usually a simple cause that’s easily identified with a few bedside tests, but all too often patients are told by doctors (or maybe Google) that their pain is sciatica.
So what do you actually have going on? Well lumbar disc bulges and herniations will cause low back pain that can radiate down the leg. So can stenosis, or bony growth of the spine from degeneration that hits those spinal nerves as they exit the cord, before they join to become the sciatic nerve. Typically if the pain is aggravated when sitting or bending forward, you’re more likely to have a disc problem. If you’re older (at risk for stenosis), or did certain sports such as gymnastics or football (at risk for spondylolithesis), forward bending and sitting may provide relief, while standing may increase the pain. There may also be lumbar instability or trigger points in the muscles around the low back causing your pain, which can refer pain all the way down to the foot.
The good news is that all of these issues can typically be effectively be treated with conservative care including chiropractic adjustments, soft tissue mobilization, and rehabilitative exercise. The biggest key is to know exactly what you’re dealing with, because what works for one of these problems may actually make another worse! Once you know what you’re dealing with you can develop an individualized care plan to get you healthy, and with an increased chance of success.
Remember, nothing beats a thorough evaluation and a correct diagnosis. Never assume, and try not to listen to Dr. Google too much.